Pink Elephants are strong advocates in the early pregnancy loss space, we don’t do this alone. Often our community supports us by sharing their personal story with key audiences. The more we amplify the different experiences of early pregnancy loss and the gaps in care the more we challenge the false narratives that exist. This in turn will lead to a different experience of loss for those who lose their babies in the future, one that is hopefully full of validation, empathy and connection ensuring no one walks the journey of pregnancy loss alone.
Catherine is one such incredible supporter of Pink Elephants; she recently spoke to a room full of Drs at a RANZCOG conference and shared her experience. Catherine was also a representative at the round table held by The Assistant Health Minister Ged Kearney in Adelaide last year sharing her experience so that she can be part of the change.
 Our Wedding Day
Our Wedding Day
Here is Catherine’s and Matts experience
Today I’m going to share with you my personal experiences of unexplained infertility, recurrent miscarriage and pregnancy after loss.
I know this isn't new data for you, but just a reminder: 1 in 4 pregnancies end in loss before 12 weeks. It is estimated that every year 100,000 to 150,000 Australians experience an early pregnancy loss. In saying that i would like to acknowledge that many of your will have had your own personal experiences of miscarriage. Please know that what i'm sharing today is personal to myself and my husband, that there is no right or appropriate way to cope with loss.
Over the past 6 years I’ve been pregnant 8 times. My husband and I are very lucky to have welcomed one healthy baby into our family 2 years ago. But we’ve also experienced 6 miscarriages.
.JPG) Pregnancy Test for Anna her Rainbow baby - 'Excitement. Heartbreak. Debilitating anxiety'
Pregnancy Test for Anna her Rainbow baby - 'Excitement. Heartbreak. Debilitating anxiety'
Matt and I were married in October 2017, we started trying for a baby the next January and fell pregnant within about 3 months. We saw the baby and a beautiful heartbeat at around 6 weeks. Then at our first appointment with our obstetrician at 9 weeks we found that I’d suffered a missed miscarriage at around 8 weeks.
This was the most shocking and heartbreaking experience for both of us, we just had no idea what to do or how to cope. Our obstetrician and his staff were lovely, they arranged everything for us and I had my first d &c a couple of days later.
I found that the narrative around our first miscarriage really centred on how common miscarriage is, but what I really heard was that lots of people go through it so it shouldn’t be so hard for us. From all of those well meaning comments I heard that my overwhelming grief was misplaced and that perhaps I should have been a little more prepared for such an outcome. I went back to work really quickly after that first d&c, I remember thinking that our obstetrician and the hospital staff didn’t talk to me about a medical certificate or leave from work so I just assumed that I was supposed to recover physically and emotionally without any support or time off. But it didn’t quite work out like that for us, we both really struggled, my cycle became really irregular and I just didn’t get pregnant again. I didn’t really understand the grief response that I was having, I was angry and so sad, I struggled to be with my friends who were pregnant, I became anxious about my husband dying and I worried every time he left the house without me. I noticed a significant decrease in resilience in all areas of my life and I felt as though I was disappointing my work colleagues, my friends and loved ones with my inability to move on with life. Despite being told multiple times how common early pregnancy loss was, I still didn’t know where to look for support. It was a really lonely and isolating time.
We met with our Obstetrician again a few months later and started fertility treatment. We did 3 rounds of IUI, then 4 cycles of IVF, all of which failed. Our inability to conceive with intervention came as a total shock, I had assumed that IVF was a means to an end – with that end being a guaranteed baby. The repeated failure to fall pregnant despite huge effort, impact on my body and bank account was highly upsetting for me and I began to assume that it was somehow completely my fault. There seemed to be a lack of support and resources in this area to prepare us for negative outcome. After the fourth IVF cycle I then had surgery to check for endometriosis - where a tiny amount was found and removed.
I then had a chemical pregnancy, which sounds like such a simple thing – just a late period. But the reality for us was that we spent three blissful days with positive pregnancy tests and dreaming of our baby. Shortly after this, we found out that I was pregnant again. The blissful days of positive pregnancy tests were no longer quite so blissful, mostly just hard and anxiety filled days where I waited desperately for the call about blood work. I had a lot of monitoring early on, and my levels were rising really well, our Dr was very positive. So it came as another huge shock to discover only an empty sac at our 7 week scan.
Two days and another heartbreaking scan after this, I had another d&c. Our fertility specialist and obstetrician worked together to make this process as quick and seamless as possible – for which Matt and I will be forever grateful. I took a little break from work after that loss, and my fertility specialist referred us to a counselor who saw us immediately and supported us both for quite a while. She also introduced me to the Pink Elephant support network and I started using their online support services. This was the first time I had been given these resources and can’t emphasise enough how effective they were for me. The Pink Elephant Support network is an Australian not-for-profit charity that supports parents through early pregnancy loss. They have a range of support services – most of which Matt and I used. They have a peer support online network that I found really helpful and their resources for pregnancy after loss were the best that I’ve been able to find. After the endometriosis removal we stopped all fertility treatment and I fell pregnant again without intervention a couple of months later. This one finally brought our beautiful Anna.
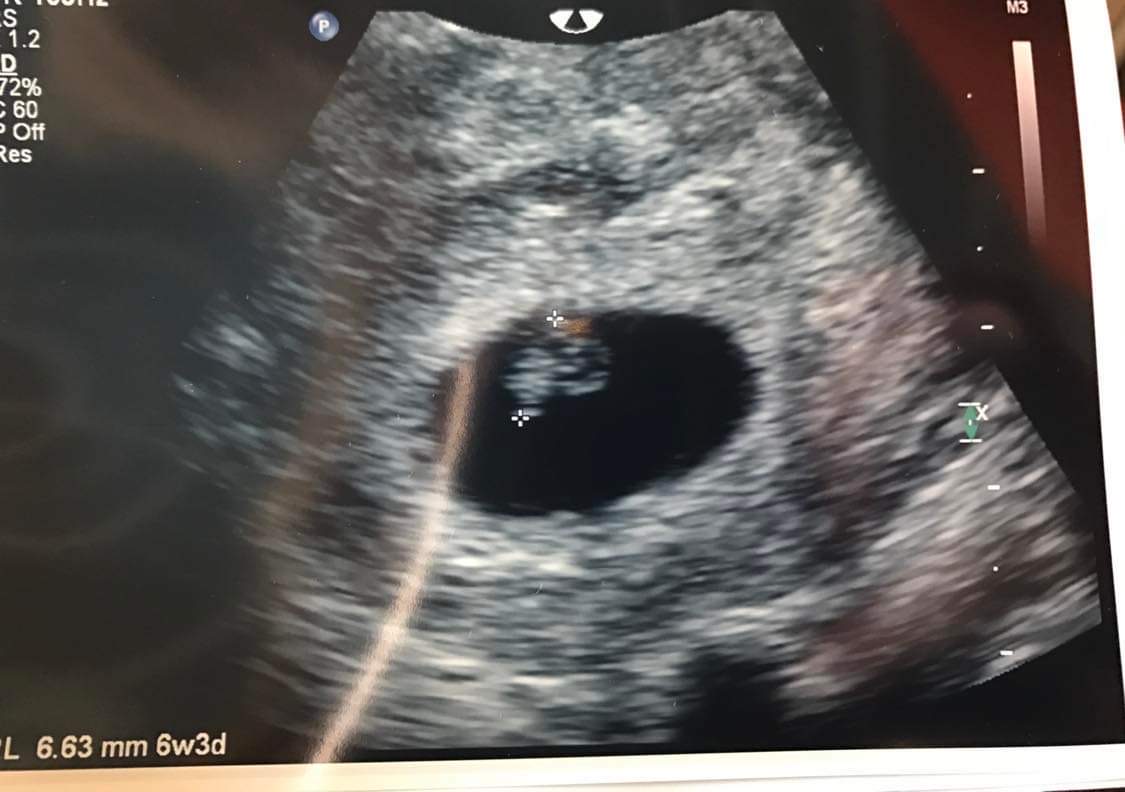 Our first precious baby with a beautiful heartbeat
Our first precious baby with a beautiful heartbeat
My pregnancy with Anna was physically a really healthy pregnancy. I was however highly anxious the whole time. The first 8 weeks of the pregnancy I was lucky to be supported by my fertility specialist and her staff who were really understanding and supportive. They let me go in for blood tests to monitor my hormones as often as I needed to and this did help to minimize my anxiety. They recognized that the first few scans were going to be terrifying for Matt and I, so they made them as easy as possible. They did this by arranging our scans at the earliest possible time, and where they could manage the timing, they didn’t make us wait, and in those first few moments of the scan they let us know what they were seeing as soon as they could. It was so helpful that they understood that that any pause in those first few moments of the scan would be hard for us. My obstetrician and his team took over my care from 9 weeks and again their understanding and support were great. I had access to midwives who I spoke to on the phone between my more formal appointments. My Obstetrician also allowed me to come in weekly to check on the baby for as long as I needed to.
But then as soon as I gave birth, it seemed like the support kind of ended. With hindsight I can recognize that I had quite bad post natal anxiety and some really terrifying intrusive thoughts. I can recognize now that my history of pregnancy loss made me a prime candidate for post natal anxiety and depression, but at the time I just thought it was part of having a newborn. Matt and I were also so deliriously happy to have brought home our healthy baby that I was willing to put up with anything if it meant that we got to keep her. Anna’s birth did coincide with another Covid outbreak and short lockdown which had an affect on the level of services that we received from CAFHS.
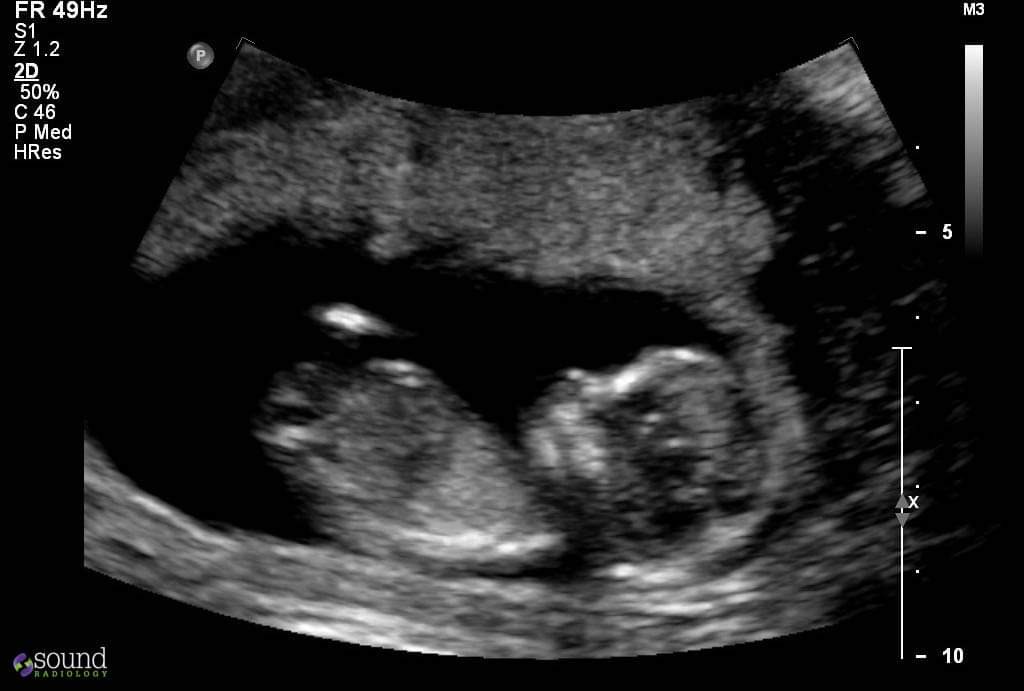 Anna our rainbow
Anna our rainbow
Since Anna’s birth in 2021 I’ve fallen pregnant four more times. The first baby made it to about 9 weeks and then its little heart just stopped. The second and third pregnancies both ended a little earlier - about 7 and 8 weeks. I’d mistakenly assumed that having my precious Anna in my arms throughout these losses would make it easier – but actually now I really know what it’s like to have a healthy pregnancy and baby, so the pain of those losses has been just as hard, sometimes harder. I had to have a d&c for each of these losses. So that’s a total of 5 d&c procedures for me and it’s this area where I’ve really y experienced a lack of support and understanding which really intensified the pain of our losses.
Undergoing a d&c is a completely heartbreaking experience. It’s generally only been a few days since I found out that my very much loved baby has died, and then I have to get myself organized to go to hospital and interact with people like it’s normal. At the hospital every time I’ve felt just like any other day surgery patient - like I’m there for a simple procedure and sent home. Sent home with no support, no resources, and no baby.
The grief is so raw at that stage, it’s hard to communicate properly. But I’ve found the majority of the staff at the hospital just don’t know what to say or how handle it, so they just ignore it.
During my most recent d&c the nurse who took me from the day surgery waiting area down to the theatre, hadn’t looked at my paperwork. So making conversation on the way there, she said brightly ‘are you ready for a nice little sleep?’ And then apologized that the wait had been so long but my Dr had been busy delivering beautiful babies all day. Once we reached the theatre and she finally opened my paperwork she was mortified and at least had the courage to apologize. But then I was back in the very common scenario of having to lessen my grief to make her feel more comfortable.
Waking up after the procedure I’m usually groggy, emotional and looking for some support. My verbal communication is affected by the anaesthetic, but while I may not be speaking clearly, I always remember exactly what I’ve said. So I remember that I’ve been crying and asking the nurses why my babies keep dying, and I remember that they don’t know what to say, so they just walk away from me. My grief was too much for them and they weren’t equipped to handle it.
So to wrap up briefly, in my experience there are a few things that the professionals around me have done that have helped and some that have made things a little harder and a little sadder.
So just a couple of things that I hope you can take away:
- With your patients experiencing pregnancy loss or pregnancy after loss, expect a grief response from them – this might look really different across patients, but
- Bereaved parents want to be met with validation that their grief matters, and especially that their much loved baby matters
- Expect a highly anxious patient and make some allowances around this where you can – such as offering more frequent blood tests and scans, and trying to limit their exposure to happy pregnant families in your waiting rooms
- Understand the anxiety response might manifest in your patient needing to ask more questions and maybe repeating questions – this isn’t about your communication and its not about them questioning your ability – its just the anxiety
- For a patient pregnant after multiple losses, the positivity after a good scan with a healthy baby and heartbeat won’t last very long. They might be lucky to make it 24 hours before the sometimes crippling anxiety is back again. If I could have lived the first trimester while being constantly attached to my Dr and ultrasound machine, I would have! Clearly this isn’t reasonable, but just expressing your understanding of that is helpful.
- Train and educate your clinic and hospital staff in communicating with patients experiencing pregnancy loss. There are resources out there to assist with this – The Pink Elephant Support Network being one of them.
- Consider some small amendments to hospital intake questions and procedures – such as not asking a d&c patient to do a pregnancy test, and managing the exposure to new mums and babies in the surgical recovery suite.
- Provide your patients with resources and access to ongoing professional support and peer support where it’s available. And please repeat this to them often – it can be hard to take on information when you’ve just been given such sad news.
And finally, to leave you with something positive, our little Anna is nearly 3 now and she is a typical busy little toddler who has quickly learnt how to push her boundaries – but she is absolutely the best thing that’s ever happened to us. I am also pregnant again with another little girl, I’m 19 weeks and with a lot of support from Louise, her team and my lovely obstetrician, I am managing my anxiety (sometimes).
 Anna in my arms
Anna in my arms
Thank you again for your time today, I hope that it’s been helpful for you to hear about our experience. I know that Matt and I are part of a lucky group of bereaved parents, and not everyone gets their Anna. So anything I can do to make the experience of others even slightly less sad than ours has been, I will keep doing.

Pink Elephant Support Network
We can’t thank Catherine enough for bravely standing up in a room full of Drs and sharing her experiences of loss. 6 miscarriages is utterly heartbreaking and we are so grateful we could be a small source of support for her but ultimately incredibly grateful that she has now chosen to walk alongside us and advocate for improved validation, empathy & understanding of early pregnancy loss in the health system.